How You Can Alleviate Patient Fears

Have Proactive Conversations to Help Patients Feel Safe
With the ongoing threat of the COVID-19 pandemic, patients continue to be reluctant to visit dental offices. Over 10% of patients – both adults and children – have delayed health care, including dental care, despite admitting the need for care.
For Dental Infection Control Awareness Month, the annual campaign from the Organization for Safety, Asepsis and Prevention (OSAP), we’re reminding you that patient communication is key to alleviating the fears that keep patients from returning to your office.
Why Is Patient Communication Important?
As the pandemic continues, many patients continue to practice caution, and may be eager to avoid places where they can’t remain masked, such as at a dental office. We don’t have to point out that patients tend to delay cleanings and regular check-ups to begin with, so the pandemic-related concerns only exacerbate the problem.
The best way to alleviate these concerns is to be proactive with communication, so patients know – even before asking – that you’re taking every precaution to keep them safe and prevent infection. So, be sure to develop a communications plan that will ensure patients receive consistent, clear, and accurate information about your infection control practices. Your outreach can include channels like social media posts, an email bulletin to patients, signage in your office itself, and perhaps most importantly, staff-patient communications.
Be Prepared to Have Candid Conversations
When you think about who spends the most time with patients, it’s often front office staff, hygienists and assistants. But the truth is, patients who have questions may approach anyone in the office. That’s why you need to be fully trained and prepared to talk with patients about the safety measures your practice is taking and any concerns they have, regardless of your role.
You should be well-versed in the latest protocols so you can answer patients’ most common questions about safety, sterilization, and anything else your patients present.
One way to keep abreast of the latest CDC guidelines pertaining to COVID and infection prevention is to make use of the Greenlight Dental Compliance Center™ by Hu-Friedy, which helps members stay up-to-date on the latest requirements.
Even if your office has a designated Infection Prevention Coordinator (IPC), consider allotting time for your team to review requirements and any changes, and then collectively update your patient communication plan. This will allow your entire team to share the most current information with patients and walk them through your processes, while also knowing they can come to the IPC with any questions they aren’t sure how to answer.
Talk to Patients About Each Step in the Process
Your patients need to be comfortable with every step your office takes to ensure their safety. If they don’t trust you, you might lose them as patients altogether.
Walk your patients through reprocessing, cleaning and sterilization, room turn-over, and the necessary PPE your staff wears during cleanings and procedures. Offer a tour of your sterilization room so they can see the sterile instruments before you open them for their visit. If you use cassettes, explain their advantages for organization and patient safety.
When it comes to helping patients become more comfortable with your safety measures and practices, there really is no such thing as too much information.
Provide Detailed Information About Your Protocols
You should be able to give patients an overview of your process to make them feel more comfortable. This includes:
Patient arrival and the office environment

Be prepared to answer the most common questions patients might ask:
- Are masks a requirement in the office?
- Does your staff wear masks?
- Is there space to social distance in your waiting room?
- Can patients bring someone with them, or do they need to arrive alone?
- Can parents and caregivers accompany their child to the exam room?
- Does your office require staff to be vaccinated against communicable diseases like COVID-19?
Infection control
Most patients don’t know much about infection control other than what they may read online. Encourage your team to initiate a conversation and proactively answer questions about the actions your office takes to protect patients, which can be an opportunity to introduce the role of the Infection Control Coordinator.
Questions to pre-emptively answer include:
- What is infection control and why this is important for health and safety at the dentist?
- What steps does your office take for infection control?
- How can patients know that the office is doing everything they need to do for infection control?
- What sterilizers or disinfectants does your office use? Are bacteria or viruses resistant to those?
- What should patients do if they become ill before their appointment?
- Are your office staff required to call out if they’re sick?
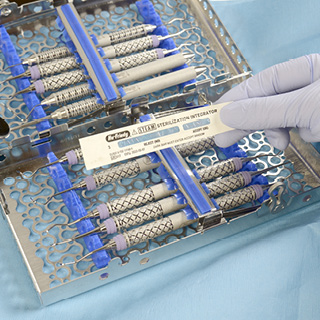
Instrument sterilization
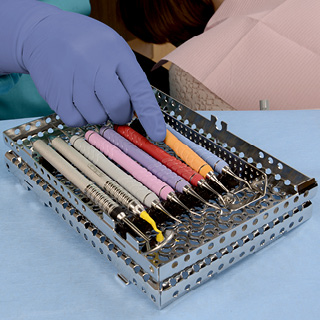
If you use an instrument management system (IMS), it can be much more reassuring to patients than a collection of loose instruments. Plus, if their instruments are neatly organized and standardized, hygienists will need to leave the room less frequently, which helps reduce patient anxiety.
Encourage your team to show patients the IMS™ Cassettes you use and explain how they work, which can answer questions patients may not know they have. Questions include:
- What does your office do with instruments after they’ve been used on patients?
- Why do you sterilize instruments between each patient?
- How does your office sterilize the instruments?
- How do patients know the instruments are actually sterile?
- What does your office do with instruments you can’t sterilize?
Surface disinfection

Lastly, be ready to answer questions about how the surfaces in your office are disinfected. During the course of treatment, lots of surfaces can potentially be contaminated from direct spray or splatter, which could lead to these types of questions from patients:
- Why are some surfaces in the office covered in plastic?
- How will patients know the surfaces not covered by plastic are clean?
- What does your office use to treat those surfaces?
It’s perfectly normal for patients to experience some fear or concern about their dental visit while COVID-19 is still an issue, but it shouldn’t stand in the way of them getting the care they need.
You’ve done the work to safeguard your office and implement best practice protocols to prevent infection and keep patients safe. Now you just have to make sure you can proactively have the conversations with patients to make them feel more comfortable about coming into the office – and leaving with a healthier smile.
