Best Practices for Hand Hygiene and Face Mask Use

Here’s What You Need to Know to Stay Protected
As of this writing, the novel respiratory illness coronavirus disease 2019 (referred to popularly as simply “coronavirus” and abbreviated as COVID-19) has spread to over 150 countries around the globe.
On January 30, the World Health Organization declared the outbreak “a public health emergency of international concern.” The U.S. Department of Health and Human Services followed suit the next day, declaring the potential spread of the new coronavirus a national health emergency. The first American deaths from the virus were reported in Washington state.
According to the World Health Organization, COVID-19 can spread person-to-person in close contact through small droplets people expel when they exhale or cough. The droplets can accumulate on surfaces, objects, and body parts, where other people can pick them up and transfer the virus into their own eyes, nose, or mouth.
Experts predicted the new virus would spread throughout most of the world, and we are seeing the global impact of infecting a significant portion of the global population. But the severity of the disease remains to be seen. We now know that the elderly and those with pre-existing medical conditions are most at risk for developing severe illnesses.
As we are watching the coronavirus play out, there’s a good chance COVID-19 will come to your community and possibly your dental practice. This is on top of the influenza virus that flares up seasonally this time of year.
Healthcare professionals – including hygienists, dental assistants, and dentists – are frontline defenders against the spread of infection, whatever form it takes. While routine dental practices are already being disrupted as part of social distancing measures, the new coronavirus is a reminder that we all must be hypervigilant about protecting our patients, colleagues, and community from the transmission of disease.
In today’s article, we’ll revisit two basic-yet-essential infection prevention best practices: the wearing of face masks and hand washing.
Proper Face Mask Use
In its 2016 “Summary of Infection Prevention Practices in Dental Settings,” the U.S. Centers for Disease Control and Prevention (CDC) says that dental healthcare professionals should wear mouth, nose, and eye protection “during procedures that are likely to generate splashes or sprays of blood or other body fluids.”
It's important to remember that in the Hierarchy of Controls for exposure to occupational hazards, personal protective equipment (PPE) like face masks are the last line of defense. That means that before evening donning a face mask, its important to focus on other control methods. For instance, during this pandemic, practices have been advised not to see patients that are experiencing symptoms of respiratory illness.
Of course, despite additional controls, face masks are a necessary part of any dental procedure. Unfortunately, bad face mask habits are common among dental professionals. And like viruses, bad habits spread rapidly. Hygienists and other dental professionals tend to take their cues from those they work with.
Here are some good face mask habits to practice and perpetuate at your dental office, starting with selecting the right mask for the task at hand.
Know How Masks Are Classified and Rated
The highest rated masks generally recommended for use in dental settings are N95 respirators, which are evaluated, tested, and approved by the National Institute for Occupational Safety and Health (NIOSH), a part of the CDC. N95 respirators filter at least 95% of airborne particles and are proscribed for use when treating patients with or suspected of having respiratory illnesses. However, most dental practices should not need N95 respirators except perhaps for emergency treatments – with proper triaging, the treatment of patients presenting with symptoms of respiratory illnesses should be postponed until a later time when they have fully recovered.
The American Society for Testing and Materials (ASTM) sets standards for the performance of and the materials used in face masks most commonly used in dental settings. The standards measure features such as fluid resistance, bacterial filtration efficiency, submicron particle filtration efficiency, differential pressure, and flame spread. Under the ASTM standards, each mask receives a rating according to its level of protection.
ASTM testing is voluntary, but the top dental mask manufacturers comply. ASTM F2100-11 standard requires a graphic display on the packaging stating the mask performance level.
Watch out for packaging that says something like “performs like a level 2.” This language may indicate the manufacturer has not actually tested their masks.
Wear Your Mask Right-Side-Up and Right-Side-Out
A dental face mask should have three layers: the outside layer is fluid-resistant, the middle layer is for filtration, and the inside layer protects your face. The inner and outer layers are not interchangeable.
Dental professionals wear their masks inside out more often than you might think. When masks are color-coded, it’s simple to tell the difference between the inside and the outside. For non-color-coded masks, check the manufacturer’s instructions. Also, manufacturers typically package their masks with the outside face up.
Dental face masks are meant to follow the contours of your face. Gaps between your skin and the edge of a mask can let contaminants in. It’s important to orient your face mask properly.
The pleats on a face mask should face down, like a waterfall.
Don (Put On) Your Mask Correctly
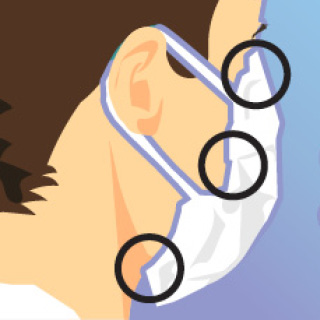
When donning their masks, most people make the mistake of looping it around their ears first. But before securing your mask, you should use your thumb to make a slight indentation or divot on the nose piece. This will help seat the mask appropriately on the bridge of your nose.
As you don your mask, open it slightly (but not so much that the folds flatten out). This will give the mask a more efficient fit.
After looping your mask around your ears, use your index and middle fingers to mold the nose piece between your eyes and across the bridge of your nose. This contoured fit helps to protect the most contaminated area on a clinician’s face.
Next, extend the mask fully over your mouth and chin. If you’re wearing a Secure Fit™ mask, adjust the lower chin strap. This will draw the outside edges of the mask securely around your face, providing 360 degrees of protection.
If you wear glasses, remove your glasses before donning your mask. Put your glasses back on after your mask.
Don’t Twist the Ear Loops Into Figure Eights
Clinicians with smaller facial structure sometimes feel as if their masks aren’t tight enough. To compensate, they shorten the ear loops by twisting them into figure eights.
The problem with that is it brings the mask material up against the mouth and nose. Condensation from the breath wets the inside of the mask, and in a process called “wicking,” causes the fibers of the mask material to swell. This, in turn, weakens the ability of the mask to filter microbes. Use of a Secure Fit mask will provide the customized fit.
Doff (Take Off) Your Mask Correctly
Just as there is a right way to put on a face mask, there’s a right way to remove one. Removing a dental face mask incorrectly risks cross-contamination. Keep in mind the outer surface of a face mask may be covered in a layer of aerosols, viruses, blood spatter, and saliva.
To doff a face mask, put your fingers underneath each of the ear loops near your ear lobes and pull straight down. Then lift the mask off and away from your face and dispose of it. Do not touch the mask itself, and do not wear a used mask outside of the treatment area. Wash or use of alcohol-based hand-rub immediately after mask removal is required.
Hand Hygiene Refresher
The CDC says, “Hand hygiene is the most important measure to prevent the spread of infections among patients and DHCP [Dental Healthcare Professionals].” Yet, the CDC also says, on average, healthcare providers clean their hands less than half the times they should.
Our article from Hand Hygiene Day 2018 covered the basic best practices for hand washing in a dental setting. But in light of COVID-19, it’s worth reviewing the main points:
Dental Professionals Should Wash Their Hands Often and Thoroughly
Potential infection is everywhere in a dental practice, from soiled dental instruments and clinical surfaces to the air itself. Everyone in your practice is at risk of catching and spreading infection, and therefore, everyone is responsible for good hygiene.
Dental professionals should wash their hands:
- At the beginning of the workday.
- Before putting on gloves.
- After removing gloves.
- Whenever gloves are torn or punctured.
- Before and after eating.
- After using the bathroom.
To wash properly, wet your hands under warm water, apply soap, and rub your hands together, hitting every part for at least 20 seconds. Rinse and dry your hands thoroughly and turn off the faucet using a disposable towel. (You may also use an alcohol-based rub instead of soap and water.)
Choose the Correct Hand Hygiene Products

Dental practices should use soap made specifically for use by dental professionals. These products will have active ingredients that have been proven to work in dental applications. They may also include moisturizers and emollients formulated to combat the effect of countless hand washings on skin.
Moisturizing your hands is more than vanity. Viruses and bacteria can easily slide into cracks and lesions in dry skin, infecting dental personnel. Plus, painful, chapped skin discourages dental professionals from practicing proper hand hygiene.
Store-bought hand lotions may contain scents that bother patients or colleagues. Petroleum-based lotions can damage latex and synthetic gloves. Choose moisturizers that have been created especially for dental professionals, such as Hand Essentials Repair Cream.
Appoint an Infection Control Coordinator
Keeping your patients, your staff, and yourself safe from infectious diseases is the job of everyone at a dental practice. But sometimes, sound habits can fall by the wayside amid the constant rush of patients and paperwork.
An infection control coordinator can make sure everyone is taking the time to wash their hands properly and is using face masks correctly. When new risks emerge, such as the new coronavirus, an infection control coordinator can spearhead the preparations for an office.
Often, the role of infection control coordinator falls to a dental assistant or dental hygienist. These clinicians are, after all, natural educators. Learn more about the role of infection control coordinator in our recent comprehensive article.
